Learn About MIPS
Reporting Requirement
Scoring Logic
Understanding Quality Payment Program
Providers may participate in the Quality Payment Program (QPP) through one of the two tracks — Merit-based Incentive Payment System (MIPS) or Advanced Alternative Payment Models (APMs).

Benefits of Quality Payment Program
- Improve the care received by Medicare beneficiaries
- Lower costs to the Medicare program through improvement of care and health
- Advance the use of healthcare information between allied providers and patients
- Educate, engage and empower patients as members of their care team
- Provide accurate, timely, and actionable performance data to clinicians, patients and other stakeholders
For 2023, Merit Based Incentive Payment System (MIPS) is divided into 4 categories

QUALITY
30%
of Total MIPS Composite Score

PROMOTING INTEROPERABILITY
30%
of Total MIPS Composite Score

IMPROVEMENT ACTIVITIES
30%
of Total MIPS Composite Score

COST
30%
of Total MIPS Composite Score
Eligibility Criteria to Participate in MIPS 2023
Eligibility: A Provider would be a MIPS eligible provider (i.e., required to report) and will receive a payment adjustment when:
- The Provider should be from the list of eligible provider types; AND
- The Provider had enrolled in Medicare before January 1, 2023; AND
- The Provider is not identified as a Qualifying APM Participant; AND
- The Provider had exceeded the low-volume threshold (exceeding all 3 low-volume elements as mentioned below)
Certified Registered Nurse Anesthetists
Clinical Nurse Specialists
Clinical Psychologists
Nurse Practitioners
Occupational Therapists
Physical Therapists
Physician
Physician Assistants
Qualified Speech-Language Pathologists
Qualified Audiologists
Registered Dietitians or Nutrition Professionals
Low-Volume Threshold Criteria for 2023:
- Bill more than $90,000 for Part B covered professional services under the Physician Fee Schedule; AND
- See more than 200 Part B patients; AND
- Provide more than 200 covered professional services to Part B patients; AND
- Minimum number of covered professional services furnished to Part B-enrolled individuals by the clinician.
General Exclusion:
- Clinicians who participate in an Advanced Alternative Payment Model (APM) entity and reach certain thresholds become Qualifying APM Participants (QPs) or Partial QPs. QPs and Partial QPs don’t need to participate in MIPS.
- MIPS eligible clinician can be excluded from participating in MIPS for the performance year if he/she is Enrolled in Medicare for the first time in the Performance year.
Eligibility for Opt-In: Eligible Providers or groups can opt-in to MIPS, if they meet or exceed at least one, but not all three, of the low-volume threshold criteria.
Eligible Provider can participate in MIPS as an Individual, Group or Virtual Group*
It is finalized that all MIPS eligible clinicians, including those in a MIPS APM, may choose to participate in MIPS as:
- An individual
- A group
- A virtual group
- An APM Entity
The APM Scoring Standard (reporting requirements and scoring approach for APM participants) will be ended beginning with the 2023 performance period.
*Definition: Virtual groups are a combination of two or more Taxpayer Identification Numbers (TINs) composed of a solo practitioner (individual MIPS eligible provider who bills under a TIN with no other NPIs billing under such TIN), or a group with 10 or fewer eligible providers under the TIN that elects to form a virtual group with at least one other such solo practitioner or group for a performance period for a year.
Beginning of Performance Period
Eligible providers can choose to participate in MIPS from January 1, 2023
- For Quality and Cost categories a full year (12-month) performance period is considered. No submission is required for the Cost category since this will be calculated by CMS.

JAN 1 2023 Starting period
- For PI and IA categories Eligible Providers can choose any 90 consecutive day time frame starting from January 1 – October 3, 2023, to report performance for.
Understanding Payment Adjustments for MIPS 2023
If an eligible provider participates in MIPS, the provider receives performance based payment adjustment according to the final score calculated from the data submitted.
The payment adjustment may be neutral, positive or negative depending upon the threshold score.
Opt-in eligible providers are also eligible to receive payment adjustments as per their performance. However, providers reporting voluntarily do receive feedback but not a payment adjustment.
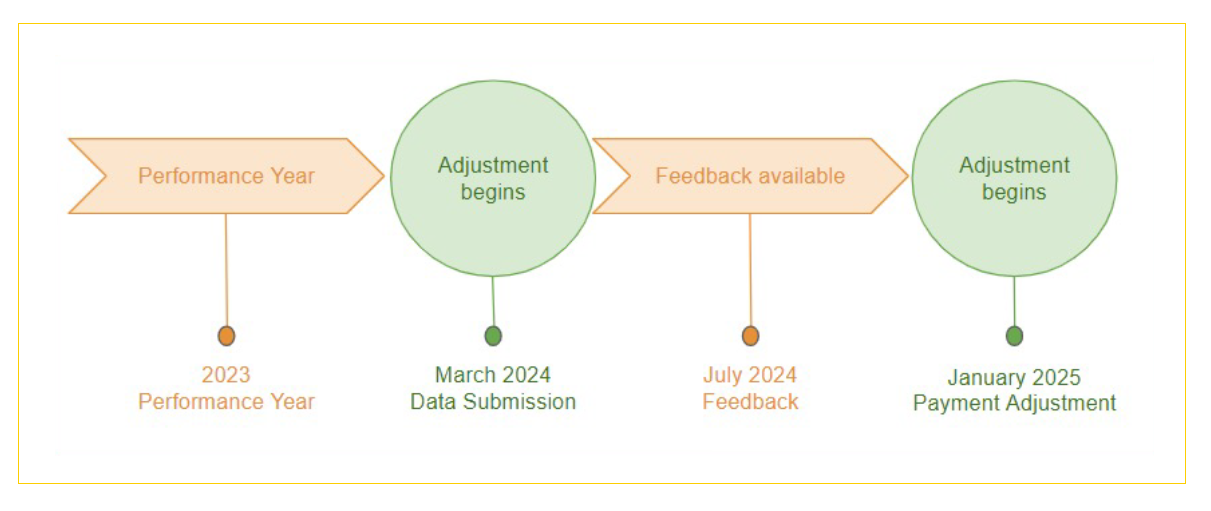
The payment adjustments are applicable to the Medicare Part B services provided 2 years after the performance year. For example, the 2023 score will be used to calculate reimbursement of Medicare Part B claims in 2025.
Payment Adjustment: Payment adjustment for the 2023 performance year ranges from – 9% to + 9% as per the CMS 2023 final rule. The scaling factor is determined in a way so that budget neutrality is achieved. The payment adjustment is applied to the amount Medicare Part B claims.
CMS has proposed to revise the complex patient bonus beginning with the 2023 MIPS performance year/2024 MIPS payment year by:
- Limiting the bonus to clinicians who have a median or higher value for at least one of the two risk indicators (HCC and dual proportion).
- Updating the formula to standardize the distribution of 2 two risk indicators so that the policy can target clinicians who have a higher share of socially and/or medically complex patients.
- Increasing the bonus to a maximum of 10.0 points.
Application of Final Score to Payment Adjustment: CMS has changed this hierarchy beginning with the 2023 performance period/2025 payment year:
- Virtual group final score
- Highest available final score from APM Entity, APP, group, and/or individual participation
Submission Types for 2023
Submission Type is the mechanism by which the submitter type submits data to CMS:
- Direct (transmitting data through a computer-to-computer interaction, such as an Application Program Interface, or API);
- Sign in and upload (attaching a file);
- Sign in and attest (manually entering data);
- Medicare Part B claims;
CMS will aggregate quality measures collected through multiple collection types. If you submit the same measure through multiple collection types, CMS will select the collection type for that measure with the greatest number of measure achievement points for scoring.
With the exception of CMS Web Interface measures, CMS will aggregate quality measures collected through multiple collection types. If you submit the same measure through multiple collection types, we will select the collection type for that measure with the greatest number of measure achievement points for scoring.

 MRO is transforming the way clinical data is exchanged...
MRO is transforming the way clinical data is exchanged...